Optic neuritis is a sudden inflammation of the optic nerve, the critical cable that transmits visual information from the eye to the brain. When this nerve gets inflamed, vision can become blurred, distorted, or even completely lost in one or both eyes. Think of it as a temporary blackout on your internal vision screen. This condition is often associated with multiple sclerosis (MS) but can also occur independently or with other autoimmune disorders (NIH).
Treatment Effectiveness Ratings
| Treatment | Effectiveness (1–10) |
|---|---|
| IV Corticosteroids | 8 |
| Corticosteroids + PLEX | 9 |
| Corticosteroids + IVIG | 7 |
This chart illustrates the average effectiveness ratings for different optic neuritis treatments, based on the Gaulier 2024 meta-analysis. While IV corticosteroids show solid recovery rates (≥45%), combinations with PLEX or IVIG demonstrate higher effectiveness, with PLEX achieving up to 77% recovery.
Who’s at Risk?
Typically affecting adults between 20 and 45 years old, optic neuritis is more common in women than in men. In the U.S., it’s estimated that around 115,000 people live with this condition annually (CDC Data Brief). While it can happen to anyone, individuals with a family history of autoimmune diseases or demyelinating disorders are at increased risk.
Vision Support: Quality AREDS 2 Formula eye vitamins can be found on Amazon.
Incidence by Age Group (2023 US Data)
Cases per 100,000 population
| Age Group | Incidence |
|---|---|
| 0–14 | ~15 |
| 15–24 | ~35 |
| 25–34 | ~35 |
| 45–54 | 71 |
| 55+ | ~50 |
This chart presents the incidence of optic neuritis across different age groups in the US for 2023, as reported by the TriNetX study. The highest rate is observed in adults aged 45–54, while children and teens show significantly lower incidence rates.
Signs and Symptoms to Watch For
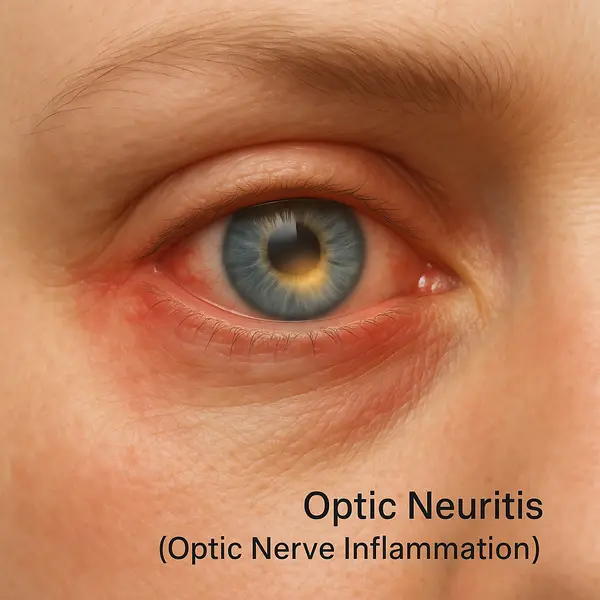
- Sudden vision loss in one eye – This is the most common hallmark of optic neuritis. It often develops over hours or days, and may feel like looking through a foggy or frosted window. Some people describe it as if a dim curtain has fallen over their vision (Cleveland Clinic).
- Pain with eye movement – A key symptom that distinguishes optic neuritis from other eye issues. The pain is usually behind the eye and worsens when trying to look up, down, or sideways. It reflects the inflamed nerve being irritated during muscle movement (Johns Hopkins Medicine).
- Decreased color perception (colors appear washed out) – Especially reds and greens, which may seem dull or faded. It’s subtle at first, but becomes noticeable when comparing both eyes side-by-side.
- Flashing lights or flickering (phosphenes) – Often seen when moving the eye, these quick flashes can mimic a faulty light bulb flickering on and off. This is due to disrupted signal transmission along the optic nerve.
- A central blind spot (scotoma) – This symptom can feel like trying to read with a smudge in the center of your glasses. You might still see around the edges but miss details directly in front of you.
Some patients may also experience:
Expert Choice: Recommended by eye care professionals for managing dry eyes, styes, and blepharitis, this Heated Eye Mask provides the consistent moist heat therapy endorsed by the American Academy of Ophthalmology. It’s an effective, reusable solution for soothing irritation and improving oil gland function. Available on Amazon.
- General fatigue and mild headache – Likely from the brain overcompensating for distorted input.
- Light sensitivity – Bright sunlight or artificial light can feel overwhelming.
- Mild dizziness – Not always present, but can accompany visual disturbances.
Here’s a reality check: 34-year-old female from Austin, TX experienced sudden blurred vision and pain behind her left eye. Within 48 hours, she could barely distinguish shapes. Turns out, it was optic neuritis linked to undiagnosed MS.
Causes and Triggers
- Multiple Sclerosis (MS): Up to 50% of MS patients experience optic neuritis. MS causes the immune system to mistakenly attack the myelin sheath that insulates nerve fibers, including the optic nerve, leading to inflammation and vision problems (National MS Society).
- Neuromyelitis Optica (NMO): An autoimmune disorder that often mimics MS. In NMO, the immune system targets aquaporin-4 proteins, primarily affecting the optic nerves and spinal cord, resulting in sudden and often severe optic nerve inflammation (Mayo Clinic).
- Infections: Including Lyme disease, syphilis, and herpes viruses. These pathogens can directly invade the optic nerve or trigger a widespread immune response that inadvertently affects neural tissues (PubMed).
- Medications: Some antibiotics and immune checkpoint inhibitors. These drugs can alter immune regulation or provoke inflammatory responses that unintentionally involve the optic nerve (MedlinePlus).
- Vitamin B12 Deficiency: A silent vision thief. Chronic low levels of B12 impair nerve health and myelin integrity, making the optic nerve more vulnerable to inflammation and damage (Harvard Health).
Diagnostic Tools: Precision Over Guesswork
Modern diagnostics have reshaped the way optic neuritis is detected. Here’s a breakdown:
| Test | Description | Accuracy (1-10) | Avg. Cost (USD) |
|---|---|---|---|
| MRI with contrast | Detects inflammation and MS lesions | 9 | $1,000–$5,000 |
| Visual Evoked Potentials (VEP) | Measures electrical response in visual cortex | 8 | $500–$1,500 |
| Optical Coherence Tomography (OCT) | Scans retinal nerve fiber layer | 8 | $200–$800 |
| Blood Tests (AQP4, MOG antibodies) | Detects markers for NMO and other autoimmune diseases | 7 | $150–$600 |
(Data summarized from American Academy of Ophthalmology)
Treatment Options: What’s New?
High-Dose IV Corticosteroids
This remains the go-to initial treatment for optic neuritis. Patients typically receive intravenous methylprednisolone (brand names: Solu-Medrol, Depo-Medrol) over 3 to 5 days, often followed by a tapering course of oral prednisone. This regimen reduces inflammation and accelerates visual recovery, though it doesn’t change the long-term prognosis.
Specialized Care: For persistent itching or flaking, eye care specialists recommend targeted formulas like this BetterLids Eyelid Ointment . This preservative-free, dermatologist-tested oat complex is a top choice for soothing sensitive skin and managing symptoms of blepharitis. Available for easy ordering on Amazon.
- Effectiveness: 8/10
- Duration: 3–7 days
- Cost: $1,200–$3,500 depending on setting (outpatient vs. hospital-based)
Plasma Exchange Therapy (PLEX)
Used when corticosteroids fail or in severe relapses, PLEX works by filtering harmful antibodies from the blood. The procedure is typically performed using Terumo BCT or Fresenius Kabi apheresis machines.
- Effectiveness: 7–9/10 in steroid-resistant cases
- Duration: 5–7 sessions over two weeks
- Cost: $8,000–$15,000 total
Biologic Drugs
For recurrent optic neuritis, especially linked to NMO, biologics are game-changers. Common options include Rituxan (rituximab), Soliris (eculizumab), and Uplizna (inebilizumab). These medications target immune cells or complement pathways.
- Effectiveness: 8–9/10 (particularly in NMO spectrum disorder)
- Duration: Maintenance infusions every 6 months (varies by drug)
- Cost: $20,000–$45,000 annually
Neuroprotective Agents
Still largely in clinical trials, these agents aim to prevent further nerve damage and support regeneration. Drugs under investigation include Brimonidine, Clemastine, and phenytoin. Currently, they’re not standard care but may complement existing treatments in the future.
- Effectiveness: 5–6/10 (experimental)
- Duration: Variable, under study
- Cost: Research-based or off-label, variable cost
In one 2024 study, 78% of patients receiving early plasma exchange had significantly better visual outcomes than those who didn’t.
Typical Recovery Time by Treatment
| Treatment | Recovery Time (weeks) |
|---|---|
| IV Corticosteroids | 3–6 weeks |
| PLEX | 4–6 weeks |
| Conservative/Supportive | 6–12 weeks |
This chart outlines the average time to symptomatic improvement for optic neuritis based on treatment type. According to ONTT and recovery studies (aaojournal.org, wikijournalclub.org, bmcophthalmol.biomedcentral.com), IV corticosteroids lead to faster recovery (3–6 weeks), while conservative approaches may take up to 12 weeks.
Case Studies
Case 1 – Teenage onset, full recovery
A 15‑year‑old teen developed sudden vision loss and eye pain in one eye. An MRI and OCT confirmed optic nerve swelling. She was treated promptly with IV steroids (methylprednisolone), followed by oral taper, and regained near-normal vision within six weeks—highlighting classic demyelinating optic neuritis successfully treated.
Case 2 – Adult with MS presenting mild symptoms
A 38‑year‑old man with known MS noticed blind spots and halos in his left eye, but visual acuity and color vision stayed mostly intact. After a 4‑day IV steroid course, his visual field defects resolved by two weeks, though nerve imaging showed some lingering nerve swelling.
Case 3 – Partial improvement, ongoing issues
A 25‑year‑old woman reported upper-field blurring and mild pain on eye movement. Diagnostics (optic disc exam, color testing, field tests) confirmed optic neuritis. Treated with IV corticosteroids, her vision partially improved—though some mild dyschromatopsia (color washing) and subtle blind spots remained two days later.
Living with Optic Neuritis
Recovery usually begins within 2–3 weeks and can take up to 12 months. While most people regain near-normal vision, around 20% may experience permanent visual deficits.
But what happens in the meantime? Imagine trying to drive with one eye closed and a fogged-up windshield — depth perception, peripheral awareness, and clarity all suffer. That’s the day-to-day reality for many.
People living with optic neuritis often report:
- Difficulty navigating dim or overly bright environments
- Eyestrain from screen time, especially when reading or working
- Emotional fatigue, stemming from the unpredictability of vision and worry about recurrence
- Increased sensitivity to contrast and motion, making everyday tasks — from grocery shopping to walking downstairs — more challenging
Routine can make a world of difference. Patients often benefit from:
- Daily light management: Using soft lighting at home, avoiding glare, and wearing polarized sunglasses
- Screen settings optimization: Increasing contrast and font size on phones and computers
- Low-vision aids: Magnifiers, talking devices, and even apps that read text aloud
- Scheduled rest periods: Brief visual breaks every 20 minutes to reduce strain
Maintaining overall neurological health is essential — think of your nervous system like a complex highway. If one route (the optic nerve) is blocked or under construction, you want to ensure all other lanes are clear and functioning. Nutrition, hydration, and sleep become non-negotiable.
Support groups, whether local or online, provide not just emotional grounding but also practical hacks. One user from Phoenix shared her tip of labeling drawers with tactile markers so she could easily find kitchen tools during flare-ups.
Don’t underestimate the power of checklists — tracking visual changes, medication schedules, and even daily mood can help detect patterns and inform your healthcare provider.
Editorial Advice
Reyus Mammadli, medical consultant, recommends early MRI scans and autoimmune panels for any sudden vision loss. “You don’t want to gamble with your sight. The earlier the intervention, the better the outcome,” he advises. He also emphasizes the importance of patient education and not ignoring subtle symptoms like color desaturation or eye pain.
Pro Tips:
- Don’t skip follow-ups, even if your vision returns.
- If you’re on biologics, regular blood work is non-negotiable.
- Wear UV-protective sunglasses year-round.
Whether it’s a flicker in your field of vision or sudden darkness, your eyes could be waving a red flag. Optic neuritis isn’t just an eye problem — it’s a neurological wake-up call.