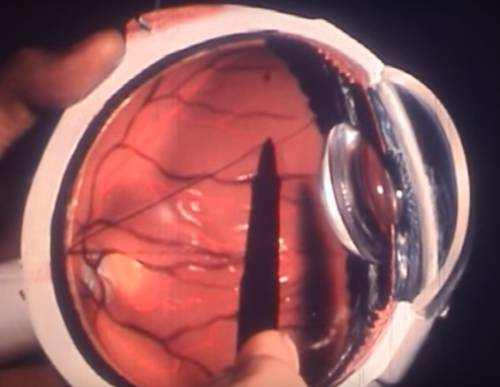
Staphylococci, streptococci, and gonococci are varieties of bacteria that cause various diseases when they enter the body. They can also be the culprit of eye diseases, such as conjunctivitis. Bacterial infections are in most cases acute and require immediate treatment.
What causes staphylococcal conjunctivitis?
Conjunctivitis is a disease of the connective tissue, which is inflammatory in nature. There are many causes of these diseases. Conventionally we can divide them into two groups: direct and indirect. The first includes bacteria, fungi, viruses, allergens. Depends on them, the form of the disease and the method of treatment. The second group of causes includes disposing factors, the presence of which significantly increases the risk of developing an ophthalmic disease of bacterial etiology. These factors include:
- weak immunity;
- Eye trauma and ingestion of foreign objects;
- Dry eye syndrome;
- Refractive errors: myopia, hypermetropia, presbyopia, astigmatism;
- contact lenses;
- blepharitis;
- Bacterial infections of ENT organs.
Very often conjunctivitis develops in people with impaired outflow of lacrimal fluid. It performs several functions, one of which is antibacterial. Germs that get into the eye are washed away by tears. With insufficient tear fluid production and constant dryness in the eye, the risk of infection increases. Bacterial conjunctivitis is often diagnosed in pregnant women against the background of hormonal malfunctions and a weakened immune system.
Vision Support: Quality AREDS 2 Formula eye vitamins can be found on Amazon.
The most common pathogens for bacterial conjunctivitis in adults are staphylococcal species, followed by Streptococcus pneumoniae and Haemophilus influenzae.
Source
Despite the presence of a large number of disposing factors, the disease is only caused by the direct impact of a pathogen on the mucosa, such as the bacterium staphylococcus in the case of bacterial conjunctivitis. Enter the same bacteria in the eye person can dirty hands, using other people’s towels, swimming in a pond with water that does not meet the hygiene requirements. In other words, in most cases, infection is a consequence of non-observance of hygiene rules. A weak immune system aggravates the situation and allows the bacteria to attack the body more aggressively. For the same reasons, streptococcal, pneumococcal, gonococcal and other types of conjunctivitis of bacterial etiology occur.
Symptoms of staphylococcal conjunctivitis
Your eyes start to chafe and watery discharge. It is practically impossible to wear glasses. The eyes become sore and watery. There is a mucous or purulent discharge on the conjunctiva. On the first or second day of the disease, the discharge is still small, but increasing afterwards. They accumulate in the conjunctival sac and trickle down through the lower edge of the eyelid. The discharge dries out during the night, which causes the eyelashes to stick together. The eye cannot be opened without the help of the hands. All these signs bother the patient for 1-2 weeks. If the treatment of streptococcal conjunctivitis is started immediately, the symptoms will disappear and the patient will fully recover.
In the absence of adequate therapy, the disease develops into a chronic form. It develops slowly. There are alternating moments of deterioration and improvement of the condition. When symptoms temporarily disappear, patients often give up on treatment. Because of this there is no complete recovery. The patient experiences the same symptoms as in acute staphylococcal conjunctivitis, but they are more moderate. There is also such a symptom as rapid eye fatigue. There is less discharge, but a detailed examination of the conjunctiva clearly shows pus or mucus. Crusts of a yellowish or light brown color may form on the eyelids.
Inflammation almost always begins in one eye. As noted above, infection occurs after direct contact of the pathogen with the mucosa. However, in most cases, the patient brings the bacteria into the second eye as well. The disease is even more difficult to tolerate. A person cannot see properly because of constant lacrimation, itching and burning. The picture becomes blurry, and it is very difficult to focus on anything. This is why immediate treatment is needed. In addition to the progression of staphylococcal conjunctivitis into a chronic form, there are other dangerous consequences of this disease, which are associated with visual impairment.
Expert Choice: Recommended by eye care professionals for managing dry eyes, styes, and blepharitis, this Heated Eye Mask provides the consistent moist heat therapy endorsed by the American Academy of Ophthalmology. It’s an effective, reusable solution for soothing irritation and improving oil gland function. Available on Amazon.
Types of bacterial conjunctivitis
Bacterial conjunctivitis can be triggered not only by staphylococcus, but also by such bacteria as pneumococcus, gonococcus, diphtheria bacillus, pseudomonas, diplobacilli and other varieties of microorganisms. Pneumococcal conjunctivitis begins acutely, the eyelids immediately swell, and red dots appear on the conjunctiva and scleral membrane as a result of multiple hemorrhages. Pus is discharged from the conjunctival sac in large quantities.
Bacterial conjunctivitis can be provoked not only by staphylococcus aureus. There is also a marginal infiltration of the cornea, which is also indicative of corneal inflammation. Pneumococcal conjunctivitis is characterized by the formation of films on the conjunctiva. They can be removed with a bandage without damaging the eye tissue. Bacteriological examination is necessary to make an accurate diagnosis. Pneumococcal infection resembles gonococcal infection. The doctor must determine the exact cause of the disease in order to correctly prescribe treatment.
Acute bacterial conjunctivitis is primary due to Staphylococcus aureus, Streptococcus pneumoniae, and Haemophilus influenzae. Other pathogens responsible for acute disease are Pseudomonas aeruginosa, Moraxella lacunata, Streptococcus viridans, and Proteus mirabilis.
Source
Gonococcal conjunctivitis is caused by Neisser’s gonococcus. Once on the connective membrane, this bacterium provokes a purulent hyperacute process. There is a significant amount of discharge from the eye. The eyelids and conjunctiva become markedly swollen and bright red. Very often keratitis, an inflammation of the stratum corneum, develops. There is a risk of ulcers forming on it. Treatment of gonococcal conjunctivitis should be started immediately.
Diphtheria bacillus rarely leads only to inflammation of the mucosa of the eye. Diphtheria of the larynx, nose, and pharynx also develop. The disease is manifested by pronounced swelling of the eyelids, copious mucopurulent discharge, and grayish films on the eyelids. They adhere tightly to the skin, so it is not recommended to remove them. After the removal of the masses, they start bleeding. During the healing process, tissue scarring occurs. Disruption of eyelash growth, eyelid curl and other complications are possible. In addition to pus and mucus, there is turbid fluid with flakes discharged from the conjunctival sac. Infection in diphtheritic conjunctivitis spreads to the cornea during the first days of the disease.
Specialized Care: For persistent itching or flaking, eye care specialists recommend targeted formulas like this BetterLids Eyelid Ointment . This preservative-free, dermatologist-tested oat complex is a top choice for soothing sensitive skin and managing symptoms of blepharitis. Available for easy ordering on Amazon.
Diprobacilli are varieties of bacteria. Some of them, such as Morax-Axenfeld’s, can lead to an inflammatory process on the conjunctiva. It occurs in a subacute or chronic form. This is one of the main differences from other conjunctivitis of a bacterial nature. The disease is accompanied by hyperemia of the eyelids in the corner of the eyes. For this reason, this pathology is also called angular, or angular conjunctivitis. The other symptoms are moderate, there is little discharge, no films or hemorrhages.
Pseudomonas conjunctivitis is rarely diagnosed. Most often it occurs due to improper use of scheduled replacement contact lenses. Such ophthalmic products should be treated with special solutions every time after removal. With their help contact optics is cleaned and disinfected. They are also stored in them, which protects it from drying out. Poor quality care for lenses or the complete absence of it becomes the cause of entry into the eye of pseudomonas bacillus, which causes inflammation of the conjunctiva. Symptoms manifest themselves quickly. The patient’s conjunctival membrane becomes swollen and very red, photophobia develops, and a cloudy white discharge appears. After some time, they become purulent. This form of conjunctivitis also risks keratitis and corneal ulceration if treatment is begun too late.
Treatment for bacterial conjunctivitis
Over-the-counter drops in pharmacies and optical salons, but without consultation it is better not to use any medications, even if they have no contraindications and are not accompanied by side effects, as the listed moisturizing solutions. Furacilin, “manganese”, boric acid are prescribed for eye irrigation.
Treatment of bacterial conjunctivitis is always carried out with the use of antibacterial drops of local action: “Floxal”, “Ciprofloxacin”. Antiseptics are also used: “Okomistin”, “Sulfacyl sodium”. Eye drops or ointments are usually used. With gonobrenorrhea, a prescription is also written for some systemic drug: “Penicillin” is prescribed intramuscularly, and “Quinolone” in tablets. Diphtheria is treated with anti-diphtheria serums, detoxifying drugs. Treatment of conjunctivitis caused by Diplobacillus is carried out with strong anti-inflammatory drugs, Vitamins that strengthen the immune system. In addition, the patient should give up alcohol, tobacco smoking, junk food. A general improvement in health contributes to a more rapid treatment of conjunctivitis. Under no circumstances should hygiene be neglected. Firstly, the patient is a danger to others. Secondly, all measures should be taken to prevent the infection from spreading to the other eye. It is necessary to wash the eye several times a day.
In the acute course of the disease, it is recommended that this be done at least 6-8 times a day. Hands may be washed with soap and water even more often. Use only disposable wipes. Pipettes should be boiled every day. The same applies to sticks intended for putting ointments on the conjunctiva. Do not interrupt treatment after symptoms are relieved by topical medications. Acute staphylococcal and other bacterial conjunctivitis are treated for about two weeks. If you do not complete treatment, you may develop a chronic condition that recurs frequently.
Conjunctivitis treatment with folk remedies
Staphylococci, gonococci, pneumococci are bacteria that can be destroyed only by special medicines. No herbal lotions and compresses are able to cope with a bacterial infection. Do not even try to cure conjunctivitis with folk remedies. But they will help relieve some of the symptoms of the disease: burning, pain and itching. When inflammation of the conjunctivitis, eyebright, chamomile apothecary, celandine, aloe juice are used. From these plants are prepared decoctions and infusions, with which to make lotions. Apply them to the eyes only after they have cooled. Dressings are not necessary. The tissues of the eyeballs should “breathe”; otherwise this creates a favorable environment for the reproduction of germs.
What is the danger of staphylococcal conjunctivitis?
One complication has already been mentioned. Acute bacterial conjunctivitis can become chronic. This is not the worst consequence. In childhood, inflammation is dangerous because it can affect the formation of the eyeballs, i.e. become one of the causes of myopia or hyperopia, as well as the progression of these refractive anomalies.
People over the age of 40, when age-related vision problems begin, have an increased risk of glaucoma. Conjunctivitis can also contribute to this dangerous ailment. Conjunctival inflammation without treatment leads to corneal clouding, which always affects the quality of vision. Do not self-treat, disregard the doctor’s recommendations or throw the therapy away prematurely. Complications will not occur if these simple rules are followed. Conjunctivitis will pass in 2-3 weeks.