Diabetic macular ischemia (DMI) is a severe complication associated with diabetes. It is an ocular disorder that can dramatically impact an individual’s quality of life by potentially leading to substantial visual impairment or even blindness. This article provides an overview of this increasingly prevalent condition, discussing its causes, symptoms, diagnosis, and treatment options.
The Causes and Risk Factors
DMI originates from changes at the capillary level in the macular area of the eye, the part responsible for central vision. It primarily arises due to uncontrolled blood glucose levels, which trigger various biochemical and pathological changes. These changes damage the small blood vessels, or capillaries, causing insufficient blood supply to the macula.
Several risk factors contribute to DMI. The length of time a person has had diabetes, difficulty in controlling blood sugar levels, systemic hypertension, and hyperlipidemia are all associated with an amplified risk of developing this condition.
Vision Support: Quality AREDS 2 Formula eye vitamins can be found on Amazon.
Symptoms
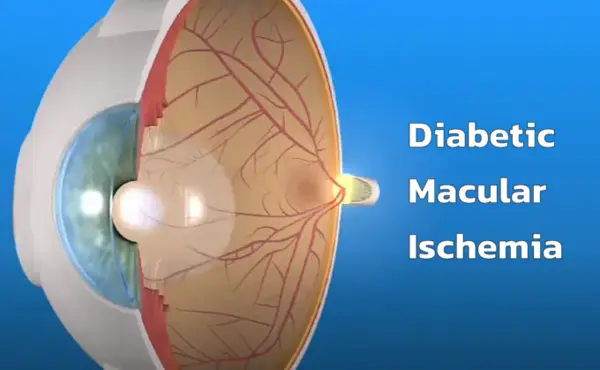
In the early stages, DMI may pose no visible symptoms. However, as the disease progresses, symptoms may start becoming more noticeable, which include:
- Decreased central vision
- Difficulty in reading
- Trouble distinguishing colors and fine details
It’s crucial to note that DMI does not cause total blindness, but it can significantly reduce central vision, making day-to-day tasks challenging.
Diagnosis
DMI’s diagnosis typically involves a comprehensive eye examination and certain specialized imaging tests. Optical coherence tomography (OCT), fluorescein angiography, and fundus photography can aid in detecting the condition. Early diagnosis can significantly slow disease progression and potentially prevent vision loss.
Treatment
No established cure for DMI exists as of now, but there are several therapeutic interventions to help manage the condition and alleviate its symptoms.
Laser photocoagulation has traditionally been used to delay the progression of macular edema. Intravitreal injections of anti-VEGF (vascular endothelial growth factor) drugs or corticosteroids can also be effective.
Expert Choice: Recommended by eye care professionals for managing dry eyes, styes, and blepharitis, this Heated Eye Mask provides the consistent moist heat therapy endorsed by the American Academy of Ophthalmology. It’s an effective, reusable solution for soothing irritation and improving oil gland function. Available on Amazon.
Maintaining tight control over blood glucose levels is paramount. This can be accomplished by adhering to a balanced diet, regular exercise, and correct medication use.
Summary
| Causes | Symptoms | Diagnosis | Treatment |
|---|---|---|---|
| High blood glucose levels | Decreased central vision | Eye examination and imaging tests | Anti-VEGF injections, laser treatment, corticosteroids |
| Duration of diabetes | Difficulty reading | OCT, fluorescein angiography, fundus photography | Proper diabetes management |
| Hypertension | Trouble distinguishing colors | – | Lifestyle changes |
| Hyperlipidemia | – | – | – |
DMI is a serious diabetic complication that needs comprehensive management and continuous monitoring. Regular eye checkups are vital for early diagnosis and effective treatment, thus helping preserve vision and minimizing the impact on quality of life.