A number of clinical, pathological, and hereditary prognostic aspects have been recognized as being associated with higher risk of establishing metastatic ocular melanoma (OM). Higher risk of metastasis is related to big tumor size, ciliary body involvement, orange pigment overlying the tumor and older patient age. Pathological findings such as epithelioid (versus spindle) morphology, is likewise related to higher risk of metastasis. Unlike melanomas of the skin, a tumor staging system is not extensively used by ocular oncologists. OM rarely spreads out through the lymph system, instead it is most likely to spread out hemotogenously, or through the blood.
Survival Rate
If melanoma is restricted in the eye only, then approximately 80% of affected individuals can make it through 5 years, whereas if ocular melanoma has actually infected distant parts, like liver then just 15% impacted people have a 5-year relative survival rate.
Prognosis
In most of the cases, it has actually been recognized that Ocular melanoma is associated with atypical mole syndrome, which is likewise known as dysplastic naevus syndrome. Dysplastic naevus syndrome and skin melanoma have likewise a great scientific amalgamation. More than 100 moles with some irregular shape and size present on their body.
The ocular melanoma has a greater incidence rate and almost 2,500 adults are evaluated in every year. It has actually been also observed that the faired skin people with blue eyes are mainly impacted by the ocular melanoma, but the cause behind this is not yet determined.
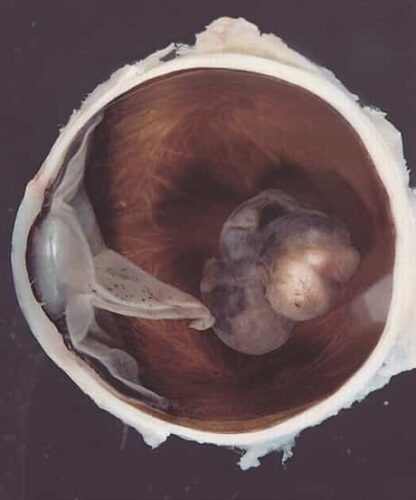
Half of the OM impacted people get impacted with metastases within 10 to 15 years after diagnosis, though sometimes, metastases is spotted even after 20-25 years after their preliminary medical diagnosis and it has been popular that metastatic condition becomes fatal for the impacted person.
The mortality rate related to half of the patients with ocular melanoma is unbothered even with the treatment development of therapeutic management of the main eye tumor. In future, more scientific and medical research needed to control the patient results.
Chromosomal Abnormality
Recent molecular genetic research study has clarified chromosomal alterations, gene expression patterns and the relationship between these patterns and total prognosis. The most extensively used predictor of metastatic disease in Europe is the detection of monosomy 3. About 20% of tumors without chromosome 3 deletion have a poor prognosis. Gains on chromosomes 6 and 8 can help fine-tune the predictive worth of monosomy 3 — gain of 6p indicating a much better prognosis and gain of 8q suggesting an even worse prognosis. This details can help predict risk of developing metastatic disease and can be acquired from a great needle biopsy at the time of treatment of the primary eye tumor.
New Gene Mutation Discovered: BAP1
It appears that the loss of chromosome 3 is related to a new genetic finding — BAP1 (BRCA associated protein 1). If BAP1 is altered or suspended in a tumor (typically found in tumors with a greater risk of metastasis) and the 2ndcopy is erased (e.g. when there is loss of one copy of chromosome 3), then this confers a higher risk of metastasis. This is a recently defined mutation and research is ongoing to understand the relationship in between this finding and treatments for OM. Remarkably, this mutation has actually likewise been recognized in a cancer called mesothelioma. Researchers in both fields are coming together to read more about this anomaly.
Gene Expression Patterns
the most commonly used predictor of metastatic disease in the United States is gene expression profiling. Using a various laboratory technique, gene expression patterns of the tumor biopsy can likewise be used to anticipate prognosis. Particularly, about half of ocular cancer malignancies are shown to be “class 1” tumors. These tumors display an unique gene expression pattern, hardly ever undergo loss of chromosome 3, and have a very low risk of metastasis. In contrast, the other half of ocular cancer malignancies fall into the “class 2” category which exhibit a various gene expression pattern, generally have lost one copy of chromosome 3, and are at an extremely high risk of metastasis.
Ocular Melanoma Metastasis
Metastatic melanoma (also called stage IV) is a general term for the dispersing of cancer beyond its original site. The liver is the most typical site of metastasis in ocular melanoma. Amongst those who establish metstatic disease, 90% of patients develop liver disease. Nevertheless, ocular melanoma can spread to any organ in the body. After the liver, common sites consist of the lung, bones and brain. Despite the fact that the cancer cells have actually spread to other parts of the body, given that the cells remain melanoma cells, this cancer is called metastatic melanoma.
Around 50% of ocular melanoma patients will establish metastatic disease within 15 years of the original medical diagnosis, and once the liver is involved, the cancer is currently incurable. Nevertheless, if metastatic disease is found early there are a few localized and systemic treatment choices that may extend life span and assistance improve lifestyle for patients.
Monitoring:
Currently, there is no consensus regarding type or frequency of scans following diagnosis and treatment of the primary eye tumor. It is necessary to talk to your physicians to decide what is right for you. Of the patients who develop metastatic disease, more than 90% of patients will develop liver metastases, the majority of surveillance methods are focused on the liver. These include: abdominal magnetic resonance imaging (MRI), abdominal ultrasound and liver function tests. The clinical community is currently working to develop standards, however up until then, each patient should take into account their specific clinical situation and discuss proper monitoring with their physicians.
