Eyelid contact dermatitis is an inflammatory response involving the eyelid skin that is triggered by contact with a trigger substance. It might be because of allergy (allergic contact dermatitis) or irritation (irritant contact dermatitis). Eyelid dermatitis is likewise called eyelid eczema.
Upper, lower or both eyelids on one or both sides can be affected by contact dermatitis The patient might report itching, stinging or burning, and the covers are red and scaly. They might swell. With persistence of the dermatitis, the eyelids become thickened with increased skin markings (lichenification). The eyelid margins may end up being involved (blepharitis). The look is comparable, whatever the cause.
Vision Support: Quality AREDS 2 Formula eye vitamins can be found on Amazon.
What Causes Eczema on Eyelids?
The thin skin of the eyelids is particularly sensitive to irritants and allergens and is hence vulnerable to develop contact dermatitis. Contact with the very same trigger may not result in a rash on other areas of skin.
How does irritant eyelid contact dermatitis occur?
Irritant contact dermatitis is a natural inflammatory reaction due to injury to the skin. Unlike allergic contact dermatitis, it does not include specific antibodies (immunoglobulins) or particular immune cells (memory T cells).
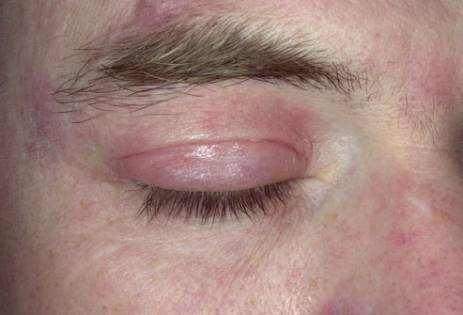
What triggers irritant eyelid contact dermatitis?
Irritant contact dermatitis might be triggered by contact with irritating substances and/or physical triggers.
Expert Choice: Recommended by eye care professionals for managing dry eyes, styes, and blepharitis, this Heated Eye Mask provides the consistent moist heat therapy endorsed by the American Academy of Ophthalmology. It’s an effective, reusable solution for soothing irritation and improving oil gland function. Available on Amazon.
Annoying substances that might cause irritant contact dermatitis of the eyelids consist of:
- Soaps and detergents
- Acids and alkalis
- Chemicals such as chlorine under safety glasses used when swimming
- Dust particles
- Hydrophobic compounds (comprised of molecules that push back water, i.e. drying agents).
- Cosmetics such as eyeliner, eye shadow, mascara and sun block.
- These substances may touch the eyelids directly or be moved from the fingers (which might be untouched by dermatitis).
Physical triggers that might cause irritant contact dermatitis consist of:
- Temperature extremes (heat or cold).
- Humidity extremes (dry or wet).
- Mechanical (rubbing or scratching).
Who gets irritant eyelid contact dermatitis?
Irritant eyelid contact dermatitis can happen in anybody. Nevertheless, it is more typical in people with sensitive skin. People with a background of atopic eczema, asthma and hayfever (“atopy”) are most likely to experience irritant contact dermatitis than people without this history.
Specialized Care: For persistent itching or flaking, eye care specialists recommend targeted formulas like this BetterLids Eyelid Ointment . This preservative-free, dermatologist-tested oat complex is a top choice for soothing sensitive skin and managing symptoms of blepharitis. Available for easy ordering on Amazon.
Any pre-existing inflammation of the skin can cause the skin’s water resistant “barrier” to be jeopardized and might make it more vulnerable to irritant contact dermatitis. Barrier function might also be malfunctioning for genetic factors.
How is the medical diagnosis of irritant eyelid contact dermatitis made?
Medical diagnosis of eyelid irritant contact dermatitis is made by identifying its characteristic functions.
An itchy rash that impacts one or both eyelids, which may take place intermittently or continuously.
Suspicion that it has actually been triggered or exacerbated by contact with an irritant (see list above).
Typically, pre-existing sensitive skin or atopic eczema.
Patch checks to thought contact allergens are negative.
It may be tough to identify the precise cause.
Allergic Eczema on Eyelids
How does allergic eyelid contact dermatitis happen?
Allergic contact dermatitis is brought on by an immune response to the trigger; this is known as the allergen. This is frequently a compound that the patient has actually been exposed to many times previously without problem. The rash typically occurs one to several days after the contact with the allergen. This can make it challenging to identify the reason for the dermatitis. Allergic contact dermatitis involves a delayed-type hypersensitivity response (likewise called type IV hypersensitivity) and includes immune memory cells.
What sets off allergic eyelid contact dermatitis?
Eyelid contact dermatitis follows direct contact with an allergen.
Allergy to cosmetics might be because of contact with allergens in:
- Emollients and moisturisers.
- Eye creams.
- Sun blocks.
- Makeups.
- Cleansers.
- Fragrances and essential oils.
- Jewellery consisting of nickel and gold.
Other prospective irritants are found in:
- Eyelash curlers or tweezers (nickel).
- Incorrect eyelashes (components or regularly, adhesives).
- Eye drops (preservatives and bactericides).
- Contact lens solution.
- Rubber goggles.
- Spectacle frames.
Eyelid eczema might likewise happen following indirect contact with an irritant, due to move of percentages of substance from the hands (through rubbing or touching the eyelids). Such irritants might include:
- Nickel from metal coins or clothes attachments.
- Fragrances.
- Nail cosmetics (varnishes and incorrect nails).
- Hair color, ie paraphenylenediamine allergy.
Eyelid contact dermatitis is sometimes activated by airborne irritants, such as allergen and plant pollens. Compositae allergy is an example of an air-borne irritant causing eyelid dermatitis.
Who gets allergic eyelid contact dermatitis?
Allergic eyelid contact dermatitis can occur in anybody. It is no more most likely in those with understood sensitive skin or atopic eczema than it is in people that have actually previously had no skin problem.
Contact allergic reaction typically develops after duplicated previous contact with the allergen, so it is not always a brand-new substance that has triggered the allergic reaction.
How is the medical diagnosis of allergic eyelid contact dermatitis made?
Diagnosis of eyelid allergic contact dermatitis is made by recognizing its particular features.
- An itchy rash that impacts one or both eyelids.
- This is probably to take place periodically at intervals of days to years.
- Suspicion that it has been triggered or exacerbated by contact with an allergen (see list above).
- Spot checks to one or more thought contact allergens are favorable.
Understanding the information of all compounds that the skin might have been exposed to in skin care, pastimes and work are a vital part of the detective work needed to discover the cause of a eyelid dermatitis. Spot tests need to be organized to develop or verify the activating irritant.
What is the treatment for eyelid contact dermatitis?
It is important to prevent contact with irritants and known or potential irritants, to ensure that the skin is healthy and able to form a waterproof barrier.
- Prevent rubbing and scratching.
- Just touch eyelids with clean, rinsed hands.
- Wash eyelids with plain water or use a cream cleanser created for sensitive skin.
- Prevent all contact with irritants identified by patch tests — this is essential life-long.
- Avoid eyelid cosmetics while the dermatitis is active.
- Wear protective wrap-round spectacles if exposed to cold, wind, dust particles and so on. Eyeglasses can likewise make it much easier to stop scratching and rubbing the eyelids.
Short courses of moderate topical corticosteroids (ie hydrocortisone 1% cream or ointment) or calcineurin inhibitors (ie pimecrolimus 1% cream) may be required to treat active inflammation. Severe contact dermatitis of the eyelids is usually treated with a brief course of oral corticosteroids.
Eyelid eczema can be followed by postinflammatory pigmentation, among the causes of dark circles under the eyes.
Treatment for Eczema on Eyelids
The skin around the eyes is thinner and more fragile than the skin of other areas of the body, making this area especially prone to annoying rashes like eczema. Also known as atopic dermatitis, true eczema is a chronic inflammatory skin problem that begins in early youth and impacts approximately 1 to 3 percent of adults, according to the American Academy of Dermatology. Eczema around the eyes can be challenging to treat due to the fact that of the sensitive tissue in this area. With severe eczema around the eyes, eyelid swelling and participation of the eye itself may impact your vision. Treatment concentrates on keeping the involved area moist, decreasing skin inflammation and preventing direct exposure to irritants. Your doctor may recommend different treatment choices based on the intensity of your eczema.
1) Moisturizers and Emollients
Eczema characteristically causes a dry, itchy, scaly rash. Your doctor will likely recommend daily use of a moisturizer, or emollient, to reduce skin dryness by forming a barrier to prevent water loss, which assists alleviate itchiness. Moisturizers also soften the skin and reduce scaling. Regular use of a moisturizer minimizes the possibility of establishing breaks in the skin, which can lead to a bacterial infection.
Ointments are the most efficient moisturizers, although their greasiness can be a downside. Your doctor may suggest a cream for daytime use and an ointment for use during the night. Moisturizers used for eye eczema differ from cosmetic moisturizers because they normally do not include any scent, sunscreen or anti-aging components. Just use a moisturizer suggested by your doctor for eye eczema.
2) Medicines to Reduce Inflammation
Your doctor may advise medication to lower the underlying skin inflammation causing eczema around your eyes. A short course of a low concentration steroid lotion or cream– such as 1 percent hydrocortisone– is typically the first option. If your interior eyelids are included, your doctor might prescribe steroid eye drops as well. Do not use an over the counter steroid cream or ointment around your eyes without first monitoring with your doctor to be sure it’s safe for you.
Although short-term treatment with topical steroid medication is often reliable for controlling eye eczema flareups, side effects can occur with long-term use. If side effects are a concern or your eye eczema does not enhance with steroid treatment, your doctor might advise another type of topical anti-inflammatory medication, such as pimecrolimus cream (Elidel) or tacrolimus lotion (Protopic). These medications are not authorized for children younger than age 2. Your doctor may advise other prescription creams, lotions, oral medications or eye drops to control your eczema.
3) Other Treatments
People with atopic dermatitis around the eyes often experience participation of other areas of the face, including the cheeks, forehead, nose and chin. Phototherapy– which involves brief bursts of exposure to a medical kind of ultraviolet light– can be beneficial if your eczema is severe and does not improve with another type of treatment. The eyes themselves should be kept closed or secured with goggles during phototherapy sessions, which generally happen 2 to 3 times per week. Numerous weeks of treatment might be needed prior to visible improvement.
Skin affected by eczema is prone to infection due to bacterial overgrowth and breaks in the skin caused by scratching or dryness. Your doctor will recommend a topical or oral antibiotic if you develop a skin infection associated to your eczema.
4) Measures to Reduce Skin Irritation
Skin impacted by eczema is easily irritated, which can make your symptoms even worse. The American Academy of Dermatology recommends limited use of a nonsoap skin cleanser, which is less drying to your skin than soap. These cleansers are hypoallergenic, fragrance-free and have a pH near that of your skin.
Preventing other potential irritants might likewise be useful, including eye makeup, nail polish and certain hair care products. If you have airborne allergic reactions, your doctor will talk with you about how to restrict your direct exposure to compounds that might exacerbate your eczema, such as pollen, dust mites and animal dander. Using a cool compress to the skin around your eyes may help temporarily decrease itchiness.
5) Specialized Care and Warnings
Because eczema around your eyes can potentially impact your vision, it’s essential to work closely with your doctor to manage your condition. Depending on the severity of your eczema and the degree to which your inner eyelids are involved, your doctor may suggest you visit an eye professional. If you have allergic reactions in addition to eczema, working with an allergist might also be handy.
Contact your doctor immediately or look for immediate healthcare if you experience any change in your vision, or experience rapidly increasing inflammation or swelling around the eyes.



