Uveitis is an inflammation of the uvea, the middle layer of the eye located between the retina and the sclera. This layer includes the iris, ciliary body, and choroid. When any of these structures become inflamed, the condition is classified as uveitis. The inflammation can be sudden (acute) or develop slowly (chronic), and if left untreated, it may lead to serious vision complications, including permanent blindness [1].
Vision Loss Risk by Uveitis Type
| Uveitis Type | Vision Loss Risk (%) |
|---|---|
| Anterior | 5% |
| Intermediate | 12% |
| Posterior | 22% |
| Panuveitis | 35% |
This chart illustrates the relative risk of vision loss associated with different types of uveitis. Anterior uveitis has the lowest associated risk, while panuveitis carries the highest, with over one-third of cases potentially leading to vision loss.
How Common Is Uveitis?
According to the Centers for Disease Control and Prevention (CDC), uveitis accounts for approximately 10% of all cases of legal blindness in the United States. It affects an estimated 121,000 people annually in the U.S. alone [2]. The condition can occur at any age but is most prevalent in individuals between 20 and 60 years old.
Vision Support: Quality AREDS 2 Formula eye vitamins can be found on Amazon.
What Causes Uveitis?
Uveitis has a wide range of potential causes, and in some cases, the exact cause remains unknown. Here are the primary culprits:
- Autoimmune diseases such as rheumatoid arthritis, ankylosing spondylitis, sarcoidosis, and lupus [3].
- Infections like herpes simplex virus (HSV), cytomegalovirus (CMV), syphilis, Lyme disease, and tuberculosis.
- Eye injuries or trauma, including post-surgical inflammation.
- Certain cancers such as lymphoma can mimic or trigger uveitis.
- Drug reactions or exposure to toxins.
Types of Uveitis
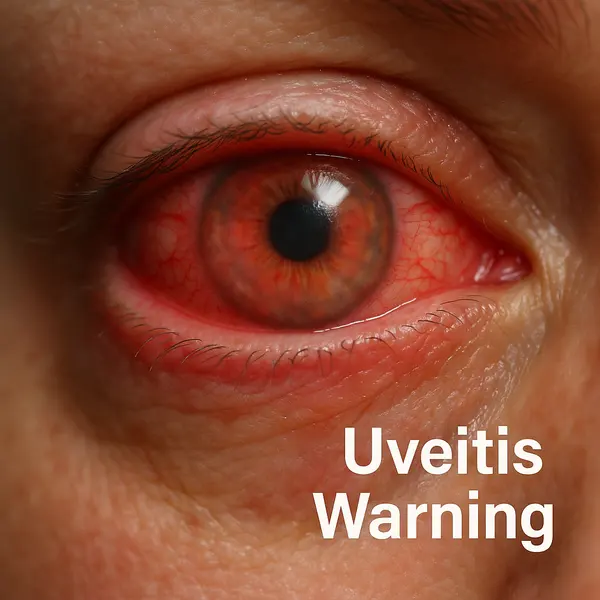
Uveitis is typically classified based on the part of the uvea affected, and each type comes with its own clinical picture, level of risk, and urgency for intervention:
- Anterior uveitis: This involves inflammation of the front part of the uvea, primarily the iris (commonly referred to as iritis). It’s the most frequently diagnosed form and, fortunately, one of the least dangerous if managed early. Patients usually experience redness, pain, and photophobia. While it can be recurrent, with regular monitoring and appropriate treatment (usually eye drops), many people live full lives with minimal disruption. Still, delaying care can lead to complications like glaucoma or cataracts.
- Intermediate uveitis: This affects the ciliary body and the vitreous, the gel-like substance in the center of the eye. It’s often less painful than anterior uveitis but comes with more floaters and mild to moderate vision changes. Although less immediately dangerous, if left untreated, it can cause complications like macular edema (swelling in the central retina). Some patients manage it with intermittent treatment, but long-term therapy may be needed in recurring cases.
- Posterior uveitis: This is a more serious form, affecting the retina and choroid. Because it impacts the structures responsible for vision processing, even mild inflammation can result in permanent vision loss if not treated quickly. Symptoms may include blurred or distorted central vision and floaters. Posterior uveitis usually requires systemic treatment, such as oral corticosteroids, immunosuppressants, or biologics, and demands close collaboration with specialists.
- Panuveitis: This is the most severe form, involving inflammation in all parts of the uvea — the iris, ciliary body, and choroid. It’s often associated with systemic autoimmune diseases and tends to cause widespread visual impairment, often rapidly. Treatment is typically aggressive and includes a combination of topical, oral, and injectable therapies. Immediate attention is crucial, as the risk of permanent blindness is significantly higher.
In short, anterior uveitis can often be managed conservatively with excellent outcomes, while posterior and panuveitis require urgent, specialized care. Intermediate uveitis sits somewhere in between — manageable, but not to be taken lightly. Understanding the type of uveitis is the first step toward protecting long-term vision and quality of life [4].
Distribution of Uveitis Types in the United States
Expert Choice: Recommended by eye care professionals for managing dry eyes, styes, and blepharitis, this Heated Eye Mask provides the consistent moist heat therapy endorsed by the American Academy of Ophthalmology. It’s an effective, reusable solution for soothing irritation and improving oil gland function. Available on Amazon.
| Uveitis Type | Prevalence (%) |
|---|---|
| Anterior uveitis | 67.3% |
| Panuveitis | 14.5% |
| Posterior uveitis | 12.6% |
| Intermediate uveitis | 5.3% |
This chart presents the prevalence of different types of uveitis in the U.S. Anterior uveitis is by far the most common form, while intermediate and posterior types account for much smaller percentages. (Source: American Academy of Ophthalmology)
Each type may present with slightly different symptoms and requires a tailored approach to diagnosis and treatment.
What Symptoms Should You Watch For?
If you’re squinting through blurry vision or tearing up more than a rom-com would justify, your eyes might be trying to tell you something serious. Uveitis can mimic other, more benign eye issues, but it tends to come with a specific set of signs — and knowing how they show up together is key.
- Eye redness: This isn’t your typical “I didn’t sleep well” redness. It often appears as a deep flush around the iris and is one of the first visible signs of anterior uveitis. If the redness is focused near the cornea and is accompanied by pain, it’s a red flag.
- Eye pain: Not just irritation — this is a persistent, sometimes throbbing discomfort that may worsen when focusing or in bright light. People often describe it as a “pressure behind the eye” or a “sore, achy” feeling.
- Blurry vision: While many conditions can cause vision to blur, in uveitis it can come on suddenly and affect one or both eyes. It may be worse in the morning or linked with floaters, which helps distinguish it from standard refractive issues.
- Sensitivity to light (photophobia): This symptom can be especially telling. Bright light may cause stabbing pain or discomfort, not just squinting. It’s more common in anterior uveitis and may force people to stay indoors or wear sunglasses constantly.
- Floaters: These are dark or shadowy spots that drift across your field of vision. While floaters can occur with age, a sudden increase — especially with other symptoms like blurred vision or pain — points to intermediate or posterior uveitis.
- Reduced visual acuity: This is not just blurring — some people experience patchy or “missing” vision, often described as gray spots or blind zones. It’s more common with inflammation in the back of the eye (posterior uveitis).
- Headache and general fatigue: Especially in autoimmune-related uveitis, systemic symptoms can accompany ocular ones. Headache behind the affected eye and fatigue may indicate broader inflammation.
While a single symptom like redness or photophobia alone may not confirm uveitis, the combination — especially when accompanied by pain and floaters — strongly suggests intraocular inflammation. If these signs persist for more than 48 hours or worsen, seeking an ophthalmologist is critical [5].
Specialized Care: For persistent itching or flaking, eye care specialists recommend targeted formulas like this BetterLids Eyelid Ointment . This preservative-free, dermatologist-tested oat complex is a top choice for soothing sensitive skin and managing symptoms of blepharitis. Available for easy ordering on Amazon.
Diagnostic Methods: How Is Uveitis Confirmed?
Diagnosing uveitis requires a thorough eye examination and sometimes a bit of medical detective work.
| Diagnostic Method | Description | Accuracy (1-10) | Average Cost (USD) |
|---|---|---|---|
| Slit-lamp examination | Allows visualization of inflammation in anterior eye segments | 9 | $100-$200 |
| Optical Coherence Tomography (OCT) | Provides cross-sectional images of the retina and choroid | 8 | $150-$300 |
| Fluorescein angiography | Highlights blood flow in the retina and choroid | 7 | $200-$500 |
| Blood tests | Identify systemic autoimmune or infectious causes | 6 | $50-$200 |
| Chest X-ray or CT scan | Detects sarcoidosis or tuberculosis-related inflammation | 7 | $100-$500 |
A comprehensive diagnosis often involves both ophthalmologists and other specialists depending on suspected underlying causes [6].
Current Treatments for Uveitis
Corticosteroids
Corticosteroids remain the cornerstone of initial uveitis treatment in the U.S. These powerful anti-inflammatory agents are most commonly prescribed in the form of topical eye drops (like Pred Forte), but moderate to severe cases may require oral prednisone or periocular injections. For chronic inflammation, steroid implants such as Retisert or Yutiq provide long-term release directly into the eye.
Typical duration: 4–12 weeks for drops; implants last up to 30 months
Effectiveness: 7–9/10, depending on location and severity
Cost: Eye drops: $50–$150/month; Retisert implant: $5,000–$7,000 per eye
Biologic Agents
For patients with autoimmune-linked uveitis, biologics are a breakthrough. Drugs such as adalimumab (Humira) and infliximab (Remicade) target specific immune pathways to reduce inflammation systemically. Approved by the FDA for non-infectious intermediate, posterior, and panuveitis, biologics are often used when corticosteroids are insufficient or contraindicated [7].
Typical duration: Long-term (months to years)
Effectiveness: 8–9/10, especially for autoimmune cases
Cost: $3,000–$6,000/month in the U.S. without assistance programs
Immunosuppressive Therapy
If steroids and biologics fall short, immunosuppressants like methotrexate, azathioprine, or mycophenolate mofetil (CellCept) are introduced. These drugs suppress the overactive immune response and help maintain long-term remission, especially in systemic conditions like sarcoidosis or Behçet’s disease.
Typical duration: 6–24 months or longer
Effectiveness: 7–8/10 with consistent monitoring
Cost: $100–$500/month (generic) + regular lab testing
Localized Steroid Implants and Devices
For chronic posterior uveitis, sustained-release intraocular implants have revolutionized care. Retisert (fluocinolone acetonide) is surgically implanted and delivers a steady dose for up to 30 months. Yutiq and Iluvien are injectable micro-implants offering similar results with less invasive delivery.
Procedure time: Outpatient; 15–30 minutes
Effectiveness: 8–9/10 for reducing recurrence and preserving vision
Cost: $4,000–$8,000 including procedure and device
Antiviral and Antibiotic Therapy
When infections are at the root of uveitis, antimicrobial treatment becomes priority. For example, valganciclovir is used for CMV retinitis, while pyrimethamine with sulfadiazine treats toxoplasmosis. Antibiotics may be combined with corticosteroids under close supervision to avoid worsening inflammation.
Typical duration: 2–6 weeks, depending on pathogen
Effectiveness: 6–8/10 when initiated promptly
Cost: $200–$2,000 depending on drug and duration
Key Treatment Considerations
Successful management of uveitis often involves a combination of therapies, regular follow-up with retinal or uveitis specialists, and cross-disciplinary care with rheumatologists or infectious disease experts. Treatment goals include preserving vision, minimizing recurrence, and preventing steroid-related side effects like cataracts and glaucoma.
Reyus Mammadli, medical consultant, advises: “Every treatment plan must be individualized. What works for autoimmune uveitis may harm in infectious cases. The earlier we match therapy to cause, the better the patient outcomes.”
Real-World Case Examples
Case 1: A 34-year-old woman from Austin, Texas, was referred to an eye clinic after weeks of persistent sensitivity to light and blurry vision. She described it as “looking through fog with a flashlight in my face.” An ophthalmologist diagnosed anterior uveitis and, after further testing, found it linked to ankylosing spondylitis. She began using corticosteroid drops and later transitioned to biologics. Her flare-ups have become rare. “I didn’t know my back pain and eye issues were connected. Now I know better — and I act fast,” she said.
Case 2: A 27-year-old man in Seattle developed floaters and flashes in both eyes. Initially brushing it off as screen fatigue, he sought help only when vision in one eye suddenly dimmed. He was diagnosed with posterior uveitis caused by latent toxoplasmosis. Treatment involved a combination of antiparasitic drugs and corticosteroids. “I thought it was just eye strain from gaming. Turns out, it was a parasite. That shook me,” he later told his physician. He now gets regular follow-ups and takes preventative medication.
Case 3: A 62-year-old retired school teacher from Des Moines had what she thought was conjunctivitis. But when redness and eye pain didn’t improve with over-the-counter drops, she saw an ophthalmologist. Intermediate uveitis was diagnosed, and chest imaging revealed previously undetected sarcoidosis. Immunosuppressants and a steroid implant brought her inflammation under control. “It took me years to see the right specialist. I wish I’d pushed for answers sooner,” she shared with her care team.
Lifestyle and Monitoring: What Else Should Patients Know?
Living with uveitis doesn’t mean life has to slow down, but it does require consistency and a bit of vigilance. Here’s what that looks like:
- Stick to follow-up visits: These appointments allow your eye doctor to monitor your progress and adjust treatment if needed. Missing them can mean missing early signs of complications.
- Use medications exactly as prescribed: Skipping doses or stopping medications early can lead to flare-ups and irreversible damage. Think of your meds like a seatbelt — they only work if you actually use them.
- Wear sunglasses to reduce photophobia: Photophobia is a heightened sensitivity to light, which can feel like a burning or stabbing pain in bright environments. Sunglasses help reduce this discomfort and protect your eyes from additional irritation.
- Avoid exposure to known infectious agents if immunosuppressed: If you’re on medications that suppress your immune system (like steroids or biologics), you’re more vulnerable to infections. This means avoiding contact with sick people, being cautious in crowded places, and practicing good hygiene.
- Report any new symptoms immediately: New floaters, flashes of light, worsening vision, or pain may signal that inflammation is returning — or that a new problem is brewing. The sooner it’s reported, the better the outcome.
Understanding these steps can make a huge difference in long-term eye health and overall well-being.
Annual Recurrence by Uveitis Type
| Uveitis Type | Annual Recurrence Rate (%) |
|---|---|
| Anterior | 24% |
| Intermediate | 18% |
| Posterior | 20% |
| Panuveitis | 27% |
This chart shows the annual recurrence rates of different uveitis types. Panuveitis has the highest recurrence rate, while intermediate uveitis shows the lowest annual return frequency.
Editorial Advice
If your eyes are inflamed, don’t blink it off. Uveitis is not your average eye irritation. With causes ranging from sneaky autoimmune conditions to serious infections, a timely and accurate diagnosis is essential.
Reyus Mammadli, medical consultant, recommends seeking an ophthalmologist at the first sign of persistent eye discomfort. “In 2025, we have the tools to prevent vision loss from uveitis, but success starts with awareness and prompt care,” he advises.
Always ask about biologics and newer implant technologies if you’re struggling with chronic or recurrent symptoms. It’s not just about seeing clearly—it’s about seeing your future with confidence.
References:
[1] American Academy of Ophthalmology. Uveitis. https://www.aao.org/eye-health/diseases/what-is-uveitis
[2] Centers for Disease Control and Prevention. https://www.cdc.gov/visionhealth/index.htm
[3] National Eye Institute. Facts About Uveitis. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/uveitis
[4] MedlinePlus. Uveitis. https://medlineplus.gov/uveitis.html
[5] Mayo Clinic. Uveitis Symptoms & Causes. https://www.mayoclinic.org/diseases-conditions/uveitis/symptoms-causes
[6] Cleveland Clinic. Uveitis Diagnosis and Treatment. https://my.clevelandclinic.org/health/diseases/17902-uveitis
[7] FDA Approval of Adalimumab for Non-infectious Uveitis. https://www.fda.gov