The lacrimal glands launch their secretions straight onto the eyeball and are therefore classified as serous kind of exocrine glands with acini secretory elements. Lacrimal gland is an important part of the lacrimal part (the lacrimal system) that plays an essential role in maintaining the normal anatomy of the eye.
Where Are the Lacrimal Glands Located?
Location of a lacrimal gland shown on the picture #1.
Vision Support: Quality AREDS 2 Formula eye vitamins can be found on Amazon.
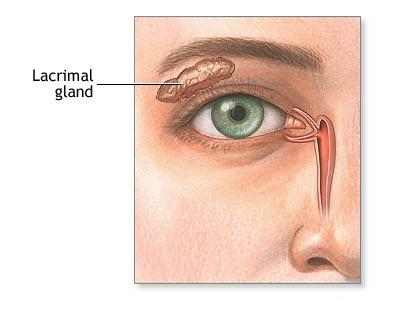
Function and Anatomy of a Lacrimal Gland
The lacrimal glands are paired, almond-shaped exocrine glands, one for each eye, that secrete the liquid layer of the tear film. They are positioned in the upper lateral area of each orbit, in the lacrimal fossa of the orbit formed by the frontal bone. Swelling of the lacrimal glands is called dacryoadenitis. The lacrimal gland produces tears which then flow into canals that connect to the lacrimal sac. From that sac, the tears drain through the lacrimal duct into the nose.
Anatomists divide the gland into two sections. The smaller palpebral portion lies close to the eye, along the inner surface area of the eyelid; if the upper eyelid is everted, the palpebral part can be seen.
The orbital part consists of great interlobular ducts that unite to form 3-5 main excretory ducts, signing up with 5– 7 ducts in the palpebral portion prior to the secreted fluid might enter upon the surface area of the eye. Tears secreted collect in the fornix conjunctiva of the upper cover, and pass over the eye surface to the lacrimal puncta, little holes found at the inner corner of the eyelids. These pass the tears through the lacrimal canaliculi on to the lacrimal sac, in turn to the nasolacrimal duct, which discards them out into the nose.
The lacrimal gland is a compound tubuloacinar gland, it is made up of many lobules separated by connective tissue, each lobule consists of numerous acini. The acini include only serous cells and produce a watery serous secretion.
Each acinus includes a grape-like mass of lacrimal gland cells with their pinnacles indicated a central lumen.
Expert Choice: Recommended by eye care professionals for managing dry eyes, styes, and blepharitis, this Heated Eye Mask provides the consistent moist heat therapy endorsed by the American Academy of Ophthalmology. It’s an effective, reusable solution for soothing irritation and improving oil gland function. Available on Amazon.
The main lumen of many of the units assemble to form intralobular ducts, and after that they unite to from interlobular ducts. The gland lacks striated ducts.
How Do Lacrimal Glands Work
The parasympathetic nerve supply originates from the lacrimatory nucleus of the facial nerve in the pons. From the pons nucleus preganglionic parasympathetic fibres run in the nervus intermedius (small sensory root of facial nerve) to the geniculate ganglion but they do not synapse there. Then, from the geniculate ganglion, the preganglionic fibers run in the greater petrosal nerve (a branch of the facial nerve) which carries the parasympathetic secretomotor fibers through the foramen lacerum, where it joins the deep petrosal nerve (which consists of postganglionic considerate fibers from the remarkable cervical ganglion) to form the nerve of the pterygoid canal (vidian nerve) which then traverses through the pterygoid canal to the pterygopalatine ganglion. Here, the fibers synapse and postganglionic fibers join the fibers of the maxillary nerve. In the pterygopalatine fossa itself, the parasympathetic secretomotor fibers branch off with the zygomatic nerve and after that branch off again, joining with the lacrimal branch of the ophthalmic part of CN V, which provides sensory innervation to the lacrimal gland in addition to the eyelid and conjunctiva.
The sympathetic postganglionic fibers originate from the exceptional cervical ganglion. They pass through as a periarteriolar plexus with the internal carotid artery, prior to they combine and form the deep petrosal nerve, which signs up with the higher petrosal nerve in the pterygoid canal. Together, higher petrosal and deep petrosal nerves form the nerve of the pterygoid canal (vidian nerve) and they reach the pterygopalatine ganglion in the pterygopalatine fossa. In contrast to their parasympathetic counterparts, sympathetic fibers do not synapse in the pterygopalatine ganglion, having done so already in the supportive trunk. However, they continue to course with the parasympathetic fibers innervating the lacrimal gland.
Specialized Care: For persistent itching or flaking, eye care specialists recommend targeted formulas like this BetterLids Eyelid Ointment . This preservative-free, dermatologist-tested oat complex is a top choice for soothing sensitive skin and managing symptoms of blepharitis. Available for easy ordering on Amazon.
Blood supply
The lacrimal artery, stemmed from the ophthalmic artery supplies the lacrimal gland. Venous blood returns via the remarkable ophthalmic vein.
Lymphatic drainage
The glands drain into the shallow parotid lymph nodes.
Nerve supply
The lacrimal nerve, derived from the ophthalmic nerve, provides the sensory part of the lacrimal gland. The higher petrosal nerve, derived from the facial nerve, supplies the parasympathetic autonomic component of the lacrimal gland. The higher petrosal nerve passes through alongside branches of the V1 and V2 divisions of the trigeminal nerve. The distance of the higher petrosal nerve to branches of the trigeminal nerve describes the phenomenon of lesions to the trigeminal nerve triggering impaired lacrimation although the trigeminal nerve does not provide the lacrimal gland.
What Happen If Lacrimal Glands Fail?
In contrast to the normal moisture of the eyes or even sobbing, there can be consistent dryness, scratching, and burning in the eyes, which are signs of dry eye syndrome (DES) or keratoconjunctivitis sicca (KCS). With this syndrome, the lacrimal glands produce less lacrimal fluid, which generally occurs with ageing or particular medications. A thin strip of filter paper (put at the edge of the eye) the Schirmer test, can be used to identify the level of dryness of the eye. Numerous medications or illness that cause dry eye syndrome can also cause hyposalivation with xerostomia. Treatment differs inning accordance with aetiology and consists of avoidance of exacerbating elements, tear stimulation and supplements, increasing tear retention, eyelid cleaning, and treatment of eye swelling.
In addition, the following can be related to lacrimal gland pathology:
- Dacryoadenitis
- Sjögren’s syndrome
Swollen Lacrimal Gland
Symptoms of Lacrimal Gland inflammation include:
- Discomfort in the area of the tear ducts
- Dry eyes
- Excessive discharge or tearing
- Inflammation of the external portion of the upper lid
- Inflammation and redness of the external part of the upper cover
- Inflammation of lymph nodes in front of the ear
- Pain in the area of inflammation
What Causes Lacrimal Gland Swelling?
Lacrimal Gland swelling might be acute or chronic. Acute swelling is triggered by a bacterial or viral infection such as mumps, Epstein-Barr infection, gonococcus and staphylococcus. Chronic swelling might be due to non-infectious inflammatory conditions such as thyroid eye condition, sarcoidosis and orbital pseudotumor.
Diagnosis
To detect Lacrimal Gland swelling, your doctor will conduct an assessment of the eyes and covers. Special diagnostic tests such as CT scan may be performed to recognize the cause of the inflammation. In specific cases, a biopsy may also be done to dismiss the existence of a lacrimal gland tumour.
Treatment for Lacrimal Gland Swelling
Based on the results of the diagnostic tests, the reason for the lacrimal gland swelling is identified. Depending on the reason for the swelling, the condition is dealt with. If the cause is a viral condition such as the mumps, your medical professional will recommend rest and warm compresses. If a more severe underlying disease is the cause, the disease will be first treated. Many patients recover completely from lacrimal gland swelling.



