Proliferative diabetic retinopathy (PDR) is a severe complication of diabetes mellitus. In this situation, damage to the retinal capillary causes the secretion of a compound called vascular endothelial development element (VEGF). VEGF triggers unusual blood vessels to grow on the surface area of the retina and elsewhere in the eye. These vessels bleed quickly and may also pull on the retina, triggering retinal traction and detachment. They typically grow to the point where they threaten vision even without the private knowing that there is anything incorrect. This is why it is so essential for diabetics to have eye examinations at routine periods.
How Is Proliferative Diabetic Retinopathy Stage Described
Oftentimes when the small capillary close down, new, unhealthy blood vessels grow. These unhealthy blood vessels are unable to feed the retina. This phase of the disease is referred to as proliferative diabetic retinopathy.
Vision Support: Quality AREDS 2 Formula eye vitamins can be found on Amazon.
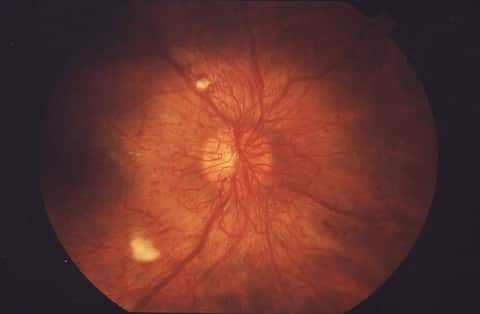
Proliferative retinopathy, an innovative kind of diabetic retinopathy, takes place when abnormal new blood vessels and scar tissue type on the surface of the retina.
The undesirable blood vessels can grow on the back of the vitreous. Vitreous is the clear jelly-like fluid that fills the majority of the eyeball. vessels might likewise bleed into the vitreous. This bleeding may trigger dark spots (floaters), hairs that look like cobwebs, or vision.
Scars from these unusual capillary sometimes pull the retina far from the back of the eye. As a result, the retina can tear or come completely loose from the eye. A detached or torn retina might lead to serious loss of sight or even blindness if it is not dealt with in time.
PDR Symptoms
When the abnormal blood vessels bleed, the blood winds up in the vitreous cavity, which is on the inside of the eye. The spots of blood may appear like little specks, bugs, or floaters. If a lot of bleeding happens, there can be a significant reduction in vision. If you have diabetes and all of a sudden see a great deal of floaters in an eye, you must notify your optometrist right away.
Expert Choice: Recommended by eye care professionals for managing dry eyes, styes, and blepharitis, this Heated Eye Mask provides the consistent moist heat therapy endorsed by the American Academy of Ophthalmology. It’s an effective, reusable solution for soothing irritation and improving oil gland function. Available on Amazon.
Another major problem of proliferative diabetic retinopathy is neovascular glaucoma. This occurs when unusual capillary grow on the iris and over the drain system of the eye (the trabecular meshwork). This can eventually result in extremely raised eye pressure, pain, inflammation, and extreme vision loss.
Treatment for Proliferative Diabetic Retinopathy
A laser treatment called panretinal photocoagulation is the main treatment for proliferative diabetic retinopathy. In this technique, wide areas of the peripheral retina are treated in a nonspecific pattern of laser spots. This alters the blood vessel circulation in the eye and enhances the shipment of oxygen to the retina. Panretinal photocoagulation minimizes the quantity of VEGF produced in the eye, which then decreases the stimulus for new unusual capillary growth. This treatment is quite extensive and frequently needs an anesthetic to avoid the laser from being too painful. Several sessions may be necessary to complete this treatment.Proliferative Diabetic Retinopathy|Vitreo Retinal Surgery, PA.
Clients have the tendency to have pain for a day or more after treatment, which is generally manageable with non-narcotic drugs. Vision is usually blurred for a week or two after treatment, and after that generally goes back to baseline. It is not rare for bleeding to occur inside the eye after treatment because it takes numerous weeks for the regression of the neovascularization to happen. Some peripheral (side) vision and some night vision may be lost as a repercussion of panretinal photocoagulation. Laser treatment for proliferative diabetic retinopathy is one of the most efficient treatments in all of medication. As an outcome, this therapy has conserved the vision of millions of clients.
Bevacizumab (Avastin) is a genetically crafted antibody versus VEGF that rapidly causes abnormal capillary to fall back. This medication can then be injected into the vitreous cavity in the office and be really useful for clients with complications from proliferative diabetic retinopathy. In basic, patients with low to moderate threat proliferative diabetic retinopathy do not require this drug, but clients with a greater danger can benefit greatly from this treatment.
Specialized Care: For persistent itching or flaking, eye care specialists recommend targeted formulas like this BetterLids Eyelid Ointment . This preservative-free, dermatologist-tested oat complex is a top choice for soothing sensitive skin and managing symptoms of blepharitis. Available for easy ordering on Amazon.
Results
In some patients, irregular capillary continue to grow and bleed in spite of great medical and laser treatment. If a patient has an extreme vitreous hemorrhage with substantial vision loss, vitrectomy surgical treatment might help treat the problem. While, if the development of unusual capillary results in tractional retinal detachment, this is a severe scenario, and surgical treatment will be necessary. In general, eyes that are followed carefully and treated early for neovascularization support and succeed for the long term. A small portion of patients have such poor blood circulation that vision is lost in spite of excellent treatment.



