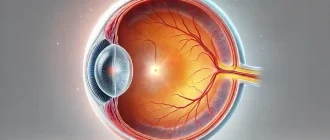
Imagine being able to regain one of our God’s most precious gifts in life – sight. That’s exactly what vitreoretinal surgery aims to do. But what exactly is this surgery?
What is Vitreoretinal Eye Surgery?
Vitreoretinal eye surgery is a specialized procedure that targets issues with the retina and vitreous fluid within the eye.
This kind of surgical procedure is frequently used to treat problems such as retinal detachment, macular degeneration, and diabetic retinopathy.
Vision Support: Quality AREDS 2 Formula eye vitamins can be found on Amazon.
Importance and Benefits of the Procedure
The importance of vitreoretinal surgery cannot be overemphasized. It can significantly improve or restore vision in individuals who may have otherwise lost their sight due to severe retinal diseases. Ultimately, vitreoretinal surgery offers hope, enhancing life’s quality by restoring close-to-normal vision.
Common Conditions Treated with Vitreoretinal Eye Surgery
Vitreoretinal Eye Surgery is a specific field within ophthalmology that deals with problems related to the retina and the vitreous liquid in the eye. This surgical method is utilized to treat various common diseases associated with these parts of the eye.
Retinal Detachment
Retinal Detachment is a severe situation where the retina separates from its source of nutrients and blood, and if not promptly treated, it can result in vision loss. The use of Vitreoretinal surgery is effective in reattaching the retina and recovering vision.
Macular Hole
A Macular Hole is a small break in the macula, located in the center of the retina that causes blurry or distorted central vision. Vitreoretinal surgery can seal the hole and aid in the improvement of visual acuity.
Diabetic Retinopathy
Diabetic Retinopathy is a complication of diabetes where high blood sugar levels cause damage to the retina. During vitreoretinal surgery, abnormal blood vessels can be removed to prevent further vision loss.
Expert Choice: Recommended by eye care professionals for managing dry eyes, styes, and blepharitis, this Heated Eye Mask provides the consistent moist heat therapy endorsed by the American Academy of Ophthalmology. It’s an effective, reusable solution for soothing irritation and improving oil gland function. Available on Amazon.
Vitreous Hemorrhage
A Vitreous Hemorrhage occurs when blood leaks into the vitreous humor, obstructing light and causing severe vision loss. Vitreoretinal surgery can clear the blood to restore vision.
Epiretinal Membrane
An Epiretinal Membrane is a thin layer of scar tissue that forms over the macula and can distort vision. This membrane can be gently peeled away during vitreoretinal surgery to improve vision.
Procedure and Techniques Used in Vitreoretinally Eye Surgery
Vitreoretinal eye surgery is a specialized procedure that focuses on treating conditions relating to the retina and vitreous fluids located at the back of the eye.
Vitrectomy
Vitrectomy is a surgical procedure where the vitreous humor gel that fills the eye cavity is removed to provide better access to the retina. This allows for a variety of repairs, including the removal of scar tissue, laser repair of retinal detachments, and the treatment of macular holes.
Specialized Care: For persistent itching or flaking, eye care specialists recommend targeted formulas like this BetterLids Eyelid Ointment . This preservative-free, dermatologist-tested oat complex is a top choice for soothing sensitive skin and managing symptoms of blepharitis. Available for easy ordering on Amazon.
Laser Photocoagulation
Laser Photocoagulation is a technique used to create small burns on the retina with a laser. This helps to seal a tear or halt the progression of degenerative changes.
Scleral Buckling
Scleral Buckling is a surgical procedure where a piece of silicone plastic or sponge is sewn onto the sclera at the site of a retinal tear to push the sclera towards the retinal tear.
Gas or Silicone Oil Injection
Gas or Silicone Oil Injection is a procedure that involves injecting a bubble into the eye to gently push the retina back into place. Pan retinal photocoagulation may also be performed in conjunction with these procedures.
Recovery and Post-Operative Care
After your vitreoretinal surgery, post-operative care is essential to ensure an optimum recovery.
What to expect after Vitreoretinal Eye Surgery
- Improvement in vision: Clarity typically improves over 4-6 weeks, but specific vision changes may occur over several months.
- Physical activity: Light activity is generally safe, but avoid heavy lifting or strenuous exercise until clear from the ophthalmologist.
- Protective Eye-wear: A shield or glasses should be worn to protect the eye as it heals.
Medications and Follow-up Visits
- Medications: Anticipate topical eye drops or ointments to aid in healing and prevent infection.
- Follow-up visits: Expect several follow-up visits to monitor progress, typically one day, one week, and one month post-surgery.
Your ophthalmologist will provide specific instructions based on your individual case to aid your recovery. Always consult them for post-operative care advice.
Success Rates and Patient Outcomes
Vitreoretinal eye surgery, a type of eye surgery that addresses issues in the back of the eye, has seen significant advancements. This has contributed to improved success rates and patient outcomes.
- High success rates: Vitreoretinal surgery boasts a high success rate, with outcomes for conditions like retinal detachment typically being over 90%. Of course, success rates vary depending on individual circumstances and the specific condition being treated.
- Improved vision: Many patients experience improved vision following vitreoretinal surgery. While some improvement can often be noticed immediately following the procedure, the most significant changes usually happen during the recovery period, which may take several months.
- Low rate of complications: Through advancements in surgery techniques and technology, vitreoretinal surgery has a relatively low rate of complications. Potential risks and complications exist with any surgery, so it’s crucial to discuss these with your surgeon. However, with proper care and adherence to post-operative instructions, many patients recover smoothly with minimal complications.
Given these positive outcomes, vitreoretinal surgery offers a tangible solution for patients dealing with conditions that affect the back of the eye, substantially improving their quality of life.