When you have a blocked tear duct, your tears cannot drain normally, leaving you with a watery, irritated eye. The condition is triggered by a partial or total obstruction in the tear drain system.
A blocked tear duct is common in newborns. The condition normally improves with no treatment during the first year of life. In adults a blocked tear duct might be because of an injury, an infection or a tumor.
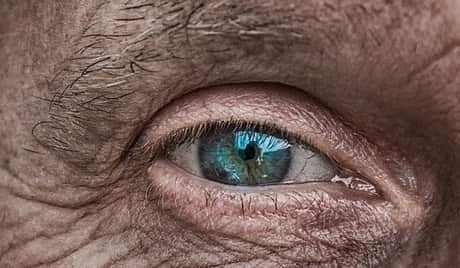
A blocked tear duct is generally correctable. Treatment depends upon the cause of the obstruction and the age of the impacted person.
Vision Support: Quality AREDS 2 Formula eye vitamins can be found on Amazon.
Blocked Tear Ducts Symptoms
Signs and symptoms of a blocked tear duct include:
- Crusting of the eyelids.
- Excessive tearing
- Painful swelling near the inside corner of the eye.
- Mucus or pus discharge from the lids and surface area of the eye.
- Blurred vision.
- Recurrent eye infection or inflammation (pink eye).
- Soreness of the white part of the eye
When to see a doctor
See your doctor if you tear constantly for numerous days or if your eye is consistently or continuously infected. A blocked tear duct may be caused by a tumor pressing on the tear drainage system. Early recognition of the tumor can give you more treatment options.
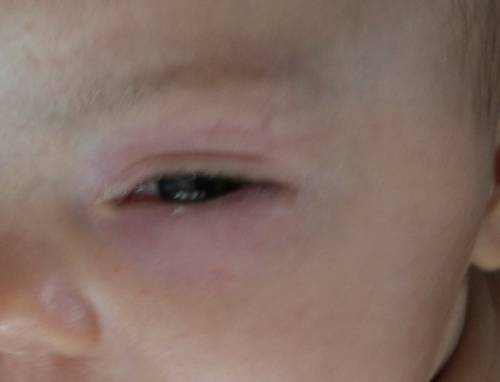
What Causes Blocked Tear Ducts?
Blocked tear ducts can take place at any age. They might even be present at birth (hereditary). Causes consist of:
- Genetic obstruction. Numerous babies are born with a blocked tear duct. The tear drainage system might not be fully developed or there might be a duct irregularity. Often a thin tissue membrane remains over the opening that clears into the nose (nasolacrimal duct).
- Age-related modifications. As you age, the small openings that drain pipes tears (puncta) might get narrower, causing clog.
- Infection or inflammation. Chronic infection or inflammation of your eyes, tear drainage system or nose can cause your tear ducts to end up being blocked.
- Injury or trauma. An injury to your face can cause bone damage or scarring near the drainage system, disrupting the normal flow of tears through the ducts. Even small particles of dirt or loose skin cells lodged in the duct can cause blockage.
- Tumor. A tumor in the nose or anywhere along the tear drainage system can cause obstruction.
Eyedrops. Seldom, long-lasting use of certain medications, such as eyedrops used to treat glaucoma, can cause a blocked tear duct. - Cancer treatments. A blocked tear duct is a possible side effect of chemotherapy medication and radiation treatment for cancer.
How the tear drainage system works?
Expert Choice: Recommended by eye care professionals for managing dry eyes, styes, and blepharitis, this Heated Eye Mask provides the consistent moist heat therapy endorsed by the American Academy of Ophthalmology. It’s an effective, reusable solution for soothing irritation and improving oil gland function. Available on Amazon.
The lacrimal glands produce most of your tears. These glands lie inside the upper lids above each eye. Normally, tears flow from the lacrimal glands over the surface area of your eye. Tears drain into the puncta, located in the within corners of your upper and lower eyelids.
Your eyelids have small canals (canaliculi) that move tears to a sac where the lids are attached to the side of the nose (lacrimal sac). From there tears take a trip down a duct (the nasolacrimal duct) draining pipes into your nose. Once in the nose, tears are reabsorbed.
An obstruction can occur at any point in the tear drainage system, from the puncta to your nose. When that occurs, your tears do not drain appropriately, giving you watery eyes and increasing your risk of eye infections and inflammation.

Who Gets Blocked Tear Ducts
Specific aspects increase your risk of developing a blocked tear duct:
Specialized Care: For persistent itching or flaking, eye care specialists recommend targeted formulas like this BetterLids Eyelid Ointment . This preservative-free, dermatologist-tested oat complex is a top choice for soothing sensitive skin and managing symptoms of blepharitis. Available for easy ordering on Amazon.
- Age and sex. Older women are at greatest risk of developing blocked tear ducts due to age-related modifications.
- Chronic eye inflammation. If your eyes are constantly irritated, red and inflamed (conjunctivitis), you’re at greater risk of developing a blocked tear duct.
- Previous surgery. Previous eye, eyelid, nasal or sinus surgery may have triggered some scarring of the duct system, potentially resulting in a blocked tear duct later on.
- Glaucoma. Anti-glaucoma medications are often used topically on the eye. If you’ve used these or other topical eye medications, you’re at higher risk of establishing a blocked tear duct.
- Previous cancer treatment. If you’ve had radiation or chemotherapy to treat cancer, particularly if the radiation was focused on your face or head, you’re at higher risk of establishing a blocked tear duct.
Is Blocked Tear Ducts Dangerous?
Since your tears aren’t draining the way they should, the tears that remain in the drain system become stagnant. This promotes development of bacteria, infections and fungis, which can result in persistent eye infections and inflammation.
Any part of the tear drain system, consisting of the clear membrane over your eye surface area (conjunctiva), can become infected or inflamed since of a blocked tear duct.
Blocked Tear Ducts Prevention
To decrease your risk of establishing a blocked tear duct later in life, get timely treatment of eye inflammation or infections. Follow these tips to prevent eye infections in the first location:
- Wash your hands completely as normal.
- Try not to rub your eyes.
- Change your eyeliner and mascara regularly. Never share these cosmetics with others.
- If you use contact lenses, keep them clean according to recommendations offered by the producer and your eye care specialist.
How Is Blocked Tear Ducts Diagnosed?
To diagnosis your condition, your doctor talks with you about your symptoms, analyzes your eyes and does a couple of tests. She or he will also examine the inside of your nose to identify if any structural conditions of your nasal passages are triggering an obstruction. If your doctor believes a blocked tear duct, she or he may have you go through other tests to find the location of the clog.
Tests used to identify a blocked tear duct consist of:
- Tear drainage test. This test measures how quickly your tears are draining. One drop of a special color is put on the surface of each eye. You may have a blocked tear duct if after five minutes the majority of the dye is still on the surface of your eye.
- Irrigation and penetrating. Your doctor may flush a saline solution through your tear drain system to check how well it’s draining pipes. Or he or she might insert a slim instrument (probe) through the tiny drainage holes at the corner of your lid (puncta) to check for blockages. In some cases this penetrating might even fix the problem.
- Eye imaging tests. For these procedures, a contrast dye is passed from the puncta in the corner of your lid through your tear drain system. Then X-ray, computerized tomography (CT) or magnetic resonance imaging (MRI) images are taken to discover the location and cause of the obstruction.
Blocked Tear Ducts Treatment
Your treatment depends on what’s triggering the blocked tear duct. You might need more than one approach to remedy the problem. If a tumor is triggering your blocked tear duct, treatment will concentrate on the reason for the tumor. Surgery may be carried out to remove the tumor, or your doctor may suggest using other treatments to diminish it.
- Medications to combat infection. If your doctor believes an infection exists, he or she might prescribe antibiotic eyedrops or pills.
- Watch-and-wait or massage. Babies born with a blocked tear duct typically get better with no treatment. This can take place as the drainage system develops during the first couple months of life. Typically a thin tissue membrane stays over the opening that empties into the nose (nasolacrimal duct). If your baby’s blocked tear duct isn’t enhancing, his/her doctor may teach you an unique massage method to assist open the membrane.
- If you’ve had a facial injury that caused blocked tear ducts, your doctor may recommend waiting a couple of months to see if the condition improves as your injury heals. As the swelling goes down, your tear ducts may end up being unblocked by themselves.
- Dilation, penetrating and flushing. For babies, this technique is done under general anesthesia. The doctor increases the size of the punctal openings with an unique dilation instrument and inserts a thin probe through the puncta and into the tear drainage system.
- For adults with partly narrowed puncta, your doctor might dilate the puncta with a small probe then flush (irrigate) the tear duct. This is a simple outpatient procedure that typically supplies at least temporary relief.
- Balloon catheter dilation. If other treatments haven’t worked or the blockage returns, this procedure may be used. It’s typically effective for babies and toddlers, and might also be used in adults with partial blockage. First the patient is given a general anesthetic. Then the doctor threads through the tear duct obstruction in the nose a tube (catheter) with a deflated balloon on the suggestion. He or she inflates and deflates the balloon a few times to open the clog.
- Stenting or intubation. This procedure is normally done using basic anesthesia. A thin tube, made of silicone or polyurethane, is threaded through one or both puncta in the corner of your eyelid. These tubes then pass through the tear drainage system into your nose. A small loop of tubing will remain visible in the corner of your eye, and the tubes are generally left in for about 3 months prior to they’re eliminated. Possible complications include inflammation from the presence of television.
Surgery
Sometimes blocked tear duct treatment requires surgery. The surgery that’s typically used to treat blocked tear ducts is called dacryocystorhinostomy (DAK-ree-oh-sis-toe-rye-nohs-tuh-me). This procedure opens the passageway for tears to drain pipes out your nose once again. First you’re offered a basic anesthetic, or a local anesthetic if it’s performed as an outpatient procedure.
The steps in this procedure vary, depending on the exact area and degree of your clog, as well as your surgeon’s experience and preferences.
- External. With external dacryocystorhinostomy, your surgeon makes an incision on the side of your nose, near where the lacrimal sac lies. After connecting the lacrimal sac to your nasal cavity and putting a stent in the new passageway, the surgeon closes up the skin cut with a couple of stitches.
- Endoscopic or endonasal. With this technique, your surgeon uses a tiny electronic camera and other tiny instruments placed through the nasal opening to your duct system. This approach needs no cut so leaves no scar. But the success rates aren’t as high similar to the external procedure.
Following surgery you’ll use a nasal decongestant spray and eyedrops to avoid infection and reduce inflammation. After 3 to 6 months, you’ll return to your doctor’s office for removal of any stents used to keep the new channel open during the healing procedure.



